
Practice Perfect 863
Plantar Fasciitis:
Treated by Gastrocnemius Recession
Plantar Fasciitis:
Treated by Gastrocnemius Recession
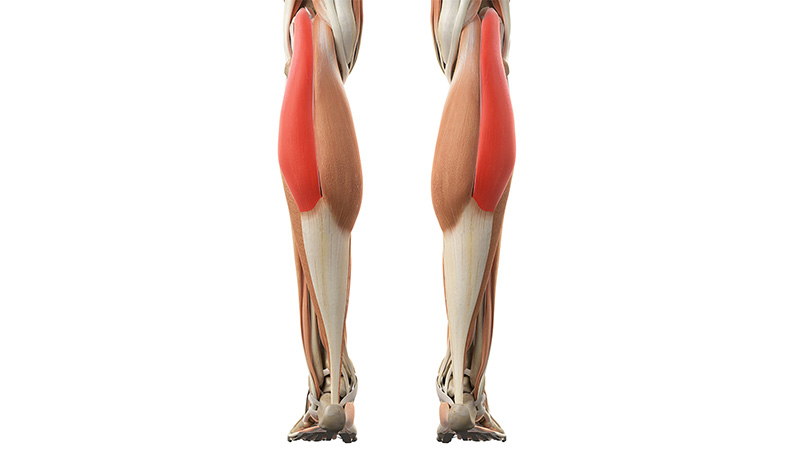
Let’s talk plantar fasciitis. Given the commonality of this disorder in the podiatric community, I have to wonder why I don’t write about it more often. However, a relatively recent systematic review by Ashad and colleagues brings the topic to the forefront.
For those who just want the bottom line and avoid further discussion:
Gastrocnemius recession is an effective treatment for plantar fasciitis.
This is not anything especially new and groundbreaking, but it brings up a few thoughts. Let’s take a quick look at the study and see where it leads us.
Arshad et al, performed a systematic review, whose inclusion criteria included randomized controlled trials (RCTs), cohorts, and case-controlled studies, isolating six studies with 118 total patients. Now, the strength of the systematic review would be stronger if it only included RCTs (actually 2 of the 6 were RCTs), so we’ll keep that in mind when considering the strength of the recommendation. The types of recessions varied (both open and endoscopic versions).
Postoperatively, ankle dorsiflexion was improved (I hope so, considering the procedure!), plantarflexion power was increased, and various pain and function scoring systems (AOFAS, VAS, SF-36) showed improvements. None of the studies had comparisons or control groups, which is difficult in surgical studies, limiting their strength. The most unfortunate part of the study, in my opinion, is that other procedures were also included in all of the studies, such as plantar fasciotomy and microdebridement. As a result, it is impossible to know how much of a treatment effect the recession itself had. As a result of these limitations, I should modify the statement above as follows:
Gastrocnemius recession, as an adjunctive procedure, is correlated with improved pain and function in patients with plantar fasciitis.
This study brings up an important point that we should focus on risk factors when treating patients with this disorder. What are those risk factors, you might ask and how does the gastrocnemius recession fit into the picture?
Riddle, et al, in a matched case control study, found obesity (BMI > 30mg/m2), lack of ankle dorsiflexion, and, spending all day at work on the feet to be three independent risk factors for plantar fasciitis2. Ankle equinus had an odds ratio of 23.3, which was the highest of the three factors.
Multiple other factors, such as poor shoe wear and a host of other biomechanical factors have also been identified as risk factors3. When you put those biomechanical factors together, it is possible to determine a unified mechanism: anything that causes strain on the plantar fascia may be implicated. This may be further honed down to specific factors that cause a pull on the fascia (ie, entities that increase the distance between the origin and insertion of the fascia). These factors include subtalar pronation, forefoot varus/supinatus, and flexible forefoot valgus. One of these is present in the vast majority of patients with plantar fasciitis and are excellent targets for treatment.
Now, given the research above about the contribution of equinus to plantar fasciitis as a significant risk factor, it makes sense that the gastrocnemius procedure would be an effective adjunctive procedure in those patients that failed nonsurgical therapy. However, with the large number of other risk factors working in combination to cause the problem, I don’t see this being a successful isolated procedure. Plantar fasciitis will always be a complex disorder requiring a multimodal treatment approach.
Best wishes.

Jarrod Shapiro, DPM
PRESENT Practice Perfect Editor
[email protected]

-
Arshad Z, Aslam A, Razzaq MA, Bhatia M. Gastrocnemius release in the management of chronic plantar fasciitis: a systematic review. Foot Ankle Int. 2022 Apr;43(4):568-575.
Follow this link -
Riddle DL, Pulisic M, Pidcoe P, Johnson RE. Risk factors for plantar fasciitis: a matched case-control study. J Bone Joint Surg Am. 2003 May;85(5):872-877.
Follow this link -
Beeson P. Plantar fasciopathy: revisiting the risk factors. Foot Ankle Surg. 2014 Sep;20(3):160-165.
Follow this link
































Comments
There are 0 comments for this article